
gentlecure: Image-Guided Superficial Radiation therapy
Musick Dermatology & Advanced Clinical Spa is proud of offer the non-surgical, gold-standard treatment for nonmelanoma skin cancer— GentleCure. GentleCure, otherwise known as Image Guided Superficial Radiation Therapy (IG-SRT), is a low-dose radiation treatment that very effectively eliminates non-melanoma skin cancer with a 99.3% cure rate. There is no need for anesthesia, minimal risk of infection or scarring, and no need for reconstructive plastic surgery. Patients heal quickly and don’t have downtime or lifestyle restrictions following treatment.
Meet Our Radiation Therapist
JoLynn is the Radiation Therapist RTT who will be with you throughout the course of treatment; safely delivering the prescribed treatment under the supervision of Dr. Musick, addressing any questions or concerns you may have, and reviewing your treatment progress with you at each treatment session. JoLynn has been a Radiation Therapist for over 26 years and has been treating patients at Musick Dermatology & Advanced Clinical Spa for almost 6 years! JoLynn is licensed in the state of Illinois and is a member of the American Registry of Radiologic Technologists and the Dermatology Association of Radiation Therapy.
Jolynn's warm demeanor and approachable nature instantly puts patients at ease, fostering a sense of calm and reassurance throughout their skin cancer journey. Her dedication to providing compassionate care makes her a cherished ally in the fight against skin cancer.

What Our Patients Have to Say
"I've been seeing Dr Musick for 2 years and I've received the best and the highest quality of care. Very professional, very personable, extraordinary staff and a special acknowledgement to Jolynn as she was exceptional as Radiation Therapist.!! The office is clean, covid free, and non-toxic. What I also value is the range of procedures both on the Dermatology side and the Cosmetic side that are modern and state of the art. I really enjoy my visits to Musick Dermatology and highly recommend his practice for Dermatology as well as Cosmetology visits!"
Am I radioactive, and is my treatment dangerous to myself or others?
No, you are not radioactive and your treatment is very safe.
Does the treatment penetrate bone?
No, the treatment only penetrates a few millimeters into the skin and has little effect on normal surrounding tissue.
How long will I be in the office each day for treatment?
Treatments generally take about 10-15 minutes total. (Simulation on the first day takes 30-45 minutes.)
How many treatments does it take?
It takes about 20 total treatments, averaging 3 treatments a week, to complete therapy.
IG-SRT Timeline
Here’s a step-by-step overview of what to expect.
Biopsy
A biopsy is performed on a suspected skin cancer in clinic with a Musick Dermatology provider.
Biopsy Results
Our staff contacts you with the results of your biopsy, identifying a skin cancer. At this point, there are typically 2 primary types of treatments: IG-SRT vs surgery (Mohs, excision). We can run a verification of benefits (VOB) while you consider your options.
Verification of Benefits (VOB)
While you are considering your options or if you decide to do IG-SRT, we will perform a VOB to identify the likely cost of this procedure based on your specific health insurance.
Decision
Once the VOB is completed, we will contact you with the estimated cost of the full procedure and arrange for any payment plans. Once you decide to go through with IG-SRT, we will schedule your simulation (sim).
Simulation (Sim)
The sim appointment is the most important part. Here, we will have you sign consent forms and discuss expectations. Photos, ultrasound images, and treatment parameters are discussed with a provider, who will then identify and mark the area of treatment. You’re ready to begin!
Treatments
Unless our Radiation Therapist is out, you will be treated by the same one at each visit. At each visit, we will determine your progress with an ultrasound, and provide treatment. Every 5 treatment visits, a provider will come in to review your case to ensure you are well on your way to being cured.
Follow-Up
After your last treatment visit, you will follow-up in six weeks for re-evaluation. At this point, we will repeat an ultrasound to ensure resolution of the skin cancer. In very rare cases, a booster may be required.
Boosters?
Boosters are additional treatment doses given over a few visits. Although fairly uncommon, the follow-up ultrasound may demonstrate a possible persisting skin cancer, which would warrant boosters.
Before & Afters
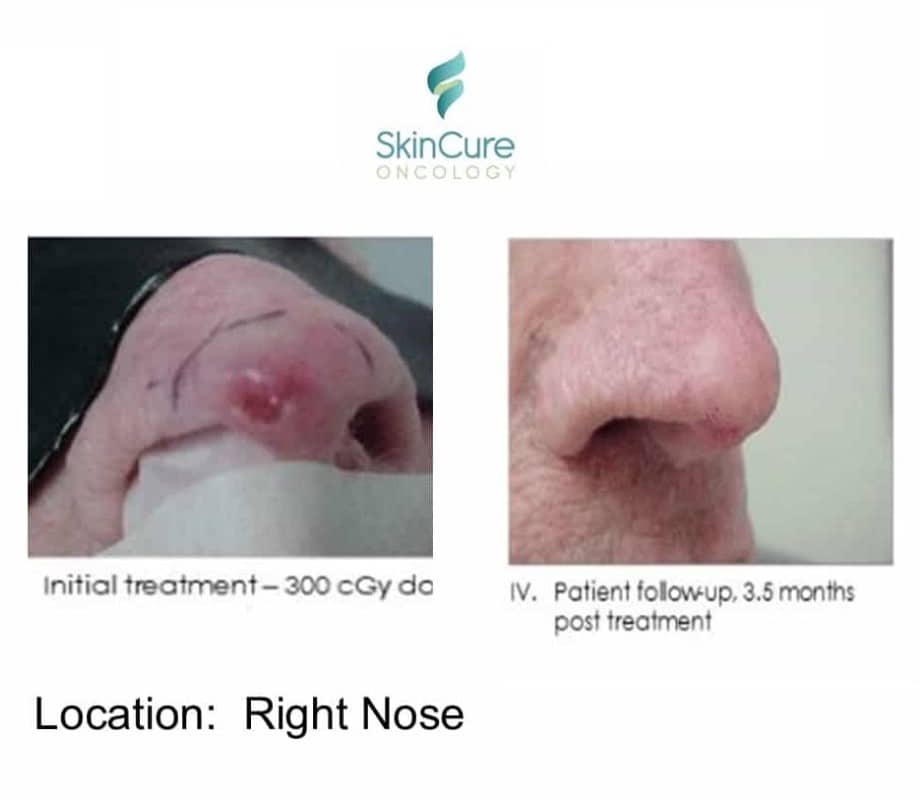
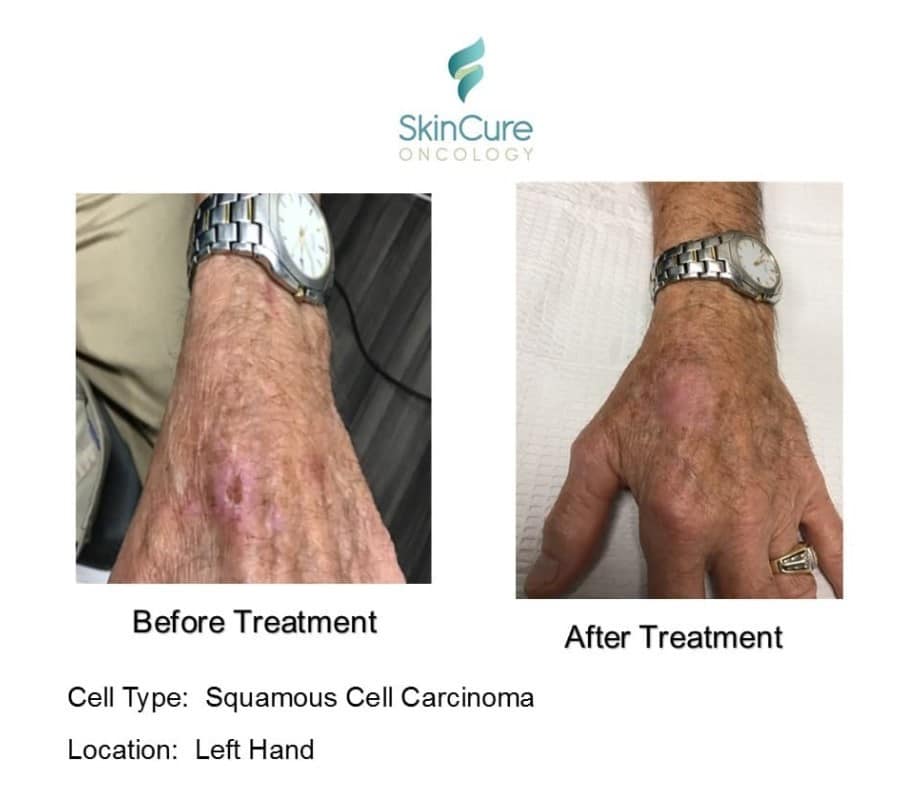
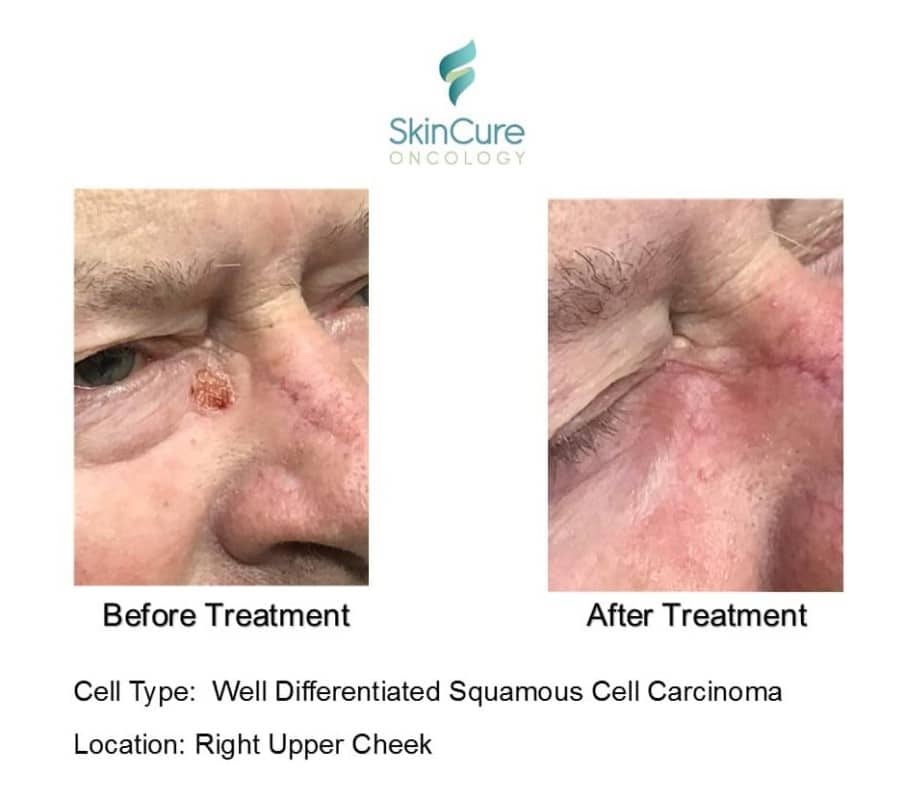
Schedule a Consultation For gentlecure Skin Cancer Treatment in IL
To learn more about SRT, contact Musick Dermatology & Advanced Clinical Spa in Swansea, IL today at 618-628-2588 ext. #5 to make an appointment. To learn more about GentleCure, please visit their website.
